Quaderns de Psicologia | 2026, Vol. 28, Nro. 1, e2219 | ISSN: 0211-3481 | 
 https://doi.org/10.5565/rev/qpsicologia.2219
https://doi.org/10.5565/rev/qpsicologia.2219

Trends in Suicide Behaviors in Valladolid During the COVID-19 Pandemic (2018-2023)
Tendencias en las conductas de suicidio en Valladolid durante la pandemia de COVID-19 (2018–2023)
Luis Sobrino Conde
Ana Isabel Segura Rodríguez
José Antonio Blanco Garrote
University Clinical Hospital of Valladolid
ABSTRACT
Objectives: The present study is conducted with the aim of analyzing trends in suicide deaths (SDs) and suicide attempts (SAs) from the years before the pandemic to the end of it. Methods: Using data on SDs and SAs collected from the Institute of Legal Medicine and the University Clinical Hospital of Valladolid, respectively, monthly incidence rates per 100,000 inhabitants were calculated, and trends were subsequently analyzed using the Joinpoint software. Results: SAs maintained the previous downward trend during the first months of the pandemic, began to increase after the first year, and stabilized a few months after the end of the pandemic. In contrast, SDs showed a pattern of stability. Conclusions: During the COVID-19 pandemic, SAs increased significantly, indicating an impact on the mental health of the population. However, this impact did not translate into an increase in SDs. More research is needed to understand the different variables involved in the development of suicide behaviors.
Keywords: Suicide; Suicide attempt; Mental health; COVID-19
RESUMEN
Objetivos: El presente estudio se realiza con el objetivo de analizar las tendencias de las muertes por suicidio (MS) y los intentos de suicidio (IS) desde los años previos a la pandemia hasta el final de la misma. Métodos: A partir de los datos de MS e IS recogidos del Instituto de Medicina Legal y del Hospital Clínico Universitario de Valladolid, respectivamente, se obtuvieron las tasas de incidencia acumuladas por 100.000 habitantes y posteriormente se analizaron las tendencias mediante el programa Joinpoint. Resultados: Los IS mantuvieron la tendencia descendente previa durante los primeros meses de pandemia, comenzaron a aumentar tras el primer año y se estabilizaron pocos meses después de su final. Por el contrario, las MS mostraron un patrón de estabilidad. Conclusiones: Durante la pandemia de COVID-19, los IS aumentaron significativamente, lo que indica un impacto en la salud mental de la población. Sin embargo, este impacto no se tradujo en un aumento de las MS. Se necesita más investigación para comprender las diferentes variables implicadas en el desarrollo de conductas de suicidio.
Palabras clave: Suicidio; Intento de suicidio; Salud mental; COVID-19
INTRODUCTION
Suicide is a serious public health problem. More than 700,000 people commit suicide each year in the world, and many more attempt it (World Health Organization, 2021). In Spain, 4,227 people committed suicide in 2022, 5.6% more than the previous year and 19% more than in 2018, making it the leading external cause of death. The most recent data provided by the Spanish National Statistics Institute (INE), belonging to the first half of 2023, confirm this trend (Instituto Nacional de Estadística, n. d.). Suicide behavior does not only refer to suicide death, as it is a multifaceted phenomenon that encompasses different manifestations ranging from ideation and planning through suicidal communication to suicide attempts and death by suicide (Al-Halabí & Fonseca-Pedrero, 2021). Although there are different conceptualizations in literature, some consensus exists in defining a suicide attempt as self-injurious behavior with inferred or actual intent to die (Turecki et al., 2019).
Suicide is a multifactorial phenomenon in which psychological, biological, and sociocultural variables interact in a continuous and dynamic way (Al-Halabí & Fonseca-Pedrero, 2021). Human behavior develops in the interaction between the characteristics of people and those of their contexts, so it is not possible to attribute this phenomenon to a single cause. Suicide behaviors must be understood in the different contexts of individuals and in the “meaning” of their suffering, as well as in their own experience of their life difficulties (Al-Halabí et al., 2021). As a multifactorial phenomenon, risk factors associated with suicide behaviors appear to have limited predictive capacity when assessed in isolation (Franklin et al., 2017). Even previous history of suicide attempts, traditionally considered as a first-order risk factor, has limited value (Ribeiro et al., 2016). Nevertheless, the identification and in-depth analysis of these factors is essential when establishing effective prevention policies.
During the last years, the world has experienced a crisis situation that may have had an impact on suicide behaviors. In January 2020, the first COVID-19 death occurred in China, and a month later, cases of infected persons had already been reported in most of the world. Spain reported its first case on January 31 in La Gomera (Islas Canarias). Since then, the number of cases increased exponentially throughout the country, leading the Government to proclaim a state of alarm on March 14. There are contradictory findings on the effects that the containment measures had on the mental health of the population, as while some studies indicate that government implementation of strict measures to reduce COVID-19 was generally effective in moderating the effects of the pandemic on mental health (Lee et al., 2021), others suggest that the lockdown policies led to a deterioration of psychological conditions (Yao et al., 2022).
Mental health problems, especially depression, are relevant risk factors for suicide. In the COVID-19 pandemic period, a widespread increase in such problems was reported across the globe (Xiong et al., 2020) with significantly higher prevalences of depression (15.97%), anxiety (15.15%), insomnia (23.87%), posttraumatic stress disorder (21.94%), and psychological distress (13.29%) (Cénat et al., 2021). Studies conducted in Spain also found higher prevalences of mental health problems (González-Sanguino et al., 2020), noting in some that up to a quarter of the people evaluated suffered from depression (27.5%), anxiety (26.9%), and stress (26.5%) (Ozamiz-Etxebarria et al., 2020).
The influence of epidemics and catastrophes on suicide behaviors has in some cases shown a seemingly paradoxical pattern, with a reduction at the beginning and a marked increase thereafter (Kõlves et al., 2013). Reductions in suicide rates have also been observed in populations that have experienced other crisis situations, such as a terrorist attack (Claassen et al., 2010) or a war (Osman & Parnell, 2015). In the case of the COVID-19 pandemic, recent meta-analyses based on data from Europe and around the world have shown that there was no widespread change in suicide trends during this period (da Cunha Varella et al., 2024; Lantos & Nyári, 2024). In addition, a time series analysis using data from 33 countries found that there was no consistent evidence that any age or sex group was differentially affected overall during the pandemic (Pirkis et al., 2022). This global pattern of stability can be observed in countries in our immediate environment, such as Portugal (Ramos et al., 2021), France (Fouillet et al., 2023) or Germany (Radeloff et al., 2022), in which no increase in suicide rates has been found with the arrival of the pandemic. However, the available evidence in Spain shows an increase in suicide deaths during the first two years of the pandemic (de la Torre et al., 2024).
While the rate of suicide deaths remained stable worldwide, the prevalence of suicidal ideation and attempts increased significantly during the pandemic in both clinical and non-clinical samples (Yan et al., 2023). Studies conducted in Spain on suicide attempts point in the same direction, showing an initial reduction in suicide-related behaviors in the first months of the pandemic and a subsequent increase (Pérez et al., 2022; Gómez-Revuelta et al., 2024).
Given the influence of the recent pandemic on mental health problems, the present study aims to analyze trends in suicide deaths (SDs) and suicide attempts (SAs) during the periods of greatest impact of the pandemic in Valladolid (Spain), as well as in the years before and after, so that we can identify critical moments that will in turn allow us to contribute to the identification of variables involved in suicide behaviors, as well as to develop more effective prevention and intervention strategies for the future appearance of similar crisis situations.
METHODS
Study Design
Descriptive retrospective cohort study.
Data Collection
The SAs data were obtained from the emergency registry of the University Clinical Hospital of Valladolid, which attended to all psychiatric emergencies and suicide attempts in the East Valladolid Health Area (258,434 inhabitants on January 1, 2023). The SDs data were collected from the Institute of Legal Medicine of Valladolid and refer to the total population of Valladolid (523,095 on January 1, 2023). We consider these data to be more reliable than those provided by the INE, since it has been shown that, in the case of Valladolid, the INE tends to underestimate the number of suicides (Giner & Guija, 2014). For both SAs and SDs, all cases registered from January 2018 to December 2023 were selected.
Data Analysis
The emergency registry of the University Clinical Hospital of Valladolid collects all the episodes in which a person has been attended in this service, so we filtered the data to select only those cases in which the reason for care was a suicide attempt. Subsequently, because some persons were attended on more than one occasion during the same month, in order to analyze monthly rates of persons attended for SAs instead of the total number of attendances made in a month for this reason, it was necessary to filter again so that each person attended was counted only once.
Monthly incidence rates per 100,000 persons were calculated for SAs and SDs. For this purpose, the monthly frequency was multiplied by 100,000, and the result was divided by the total population of the East Valladolid Health Area in the case of SAs and by the total population of Valladolid in the case of SDs. For all months of the same year, the annual population data were used (e.g., for both January and February 2018, the 2018 population was also used).
Joinpoint Trend Analysis Software (Version 5.0.2—May 2023), a statistical regression analysis software that allows the identification of months in which significant changes in the time trend (changes in the linear slope) occurred, was used to evaluate trends over time. The magnitude of the trend changes, either increase or decrease, is estimated as the Monthly Percent Change (MPC). The analysis performed by Joinpoint tests the model fit with a maximum of 7 joinpoints and determines which number of joinpoints best fit the temporal trend of the data using the Monte Carlo permutation method (Kim et al., 2000).
RESULTS
In the period from January 2018 to December 2023, 283 SDs were recorded in the province of Valladolid, resulting in an MMIR of 0.752 per 100,000 inhabitants (Table 1).
Table 1. Number of SDs and SAs, and mean monthly incidence rate (per 100,000 persons)
SDs |
SAs |
|||
N |
MMIR |
N |
MMIR |
|
2018 |
49 |
0.779 |
326 |
11.767 |
2019 |
44 |
0.704 |
323 |
11.738 |
2020 |
40 |
0.642 |
249 |
9.692 |
2021 |
45 |
0.721 |
331 |
11.752 |
2022 |
53 |
0.844 |
496 |
19.154 |
2023 |
52 |
0.823 |
504 |
19.208 |
2018-2023 |
283 |
0.752 |
2017 |
13.885 |
Note: SDs: Suicide deaths; SAs: Suicide attempts; MMIR: Mean monthly incidence rate
Figure 1 shows the evolution of the monthly incidence rate of suicides per 100,000 inhabitants together with the results of the Joinpoint regression analysis, which presents the points at which the trends in the rates change significantly, as well as the MPC of each segment. No significant trend change is observed over the 2018-2023 period, so there is a pattern of stability in SDs that does not seem to be affected by the pandemic period.
Figure 1. Suicide deaths incidence rate (100,000 person-months) in Valladolid, 2018-2023, estimated from Joinpoint regression analysis
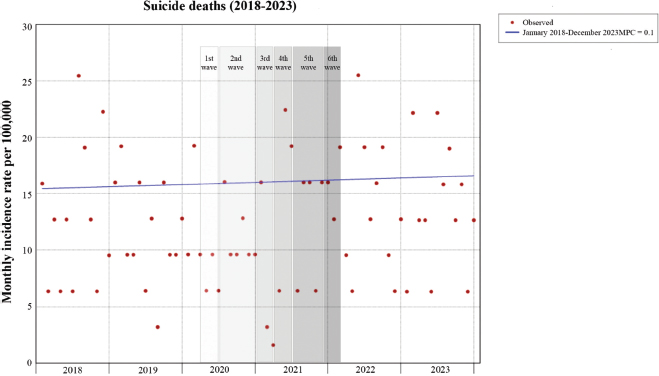
Note: *Indicates that the Monthly Percent Change (MPC) is significantly different from zero at the alpha = 0.05 level.
Regarding SAs, from 2018 to the end of 2023, 2017 persons received health care for this reason, which results in a mean monthly incidence rate of 13.885 per 100,000 inhabitants (Table 1). These statistics show that during this period, about 14 people were attended in the emergency service each month for a suicide attempt. Figure 2 shows the evolution of the monthly incidence rate together with the results of the Joinpoint regression analysis. The model that best fits the trend changes is the one with two joinpoints, the first in January 2021 and the second in September 2022. From January 2018 to January 2021, the estimated MPC = -0.70, from January 2021 to September 2022, MPC = 3.90*, and from September 2022 to December 2023, MPC = -0.34. The regression analysis reflects a slightly decreasing trend in the rate of SAs from 2018 until the beginning of the pandemic, with a significant reduction in the first months and a subsequent increase from January 2021, coinciding with the third wave of infections, which is maintained until mid-2022, when a slight decrease begins to be observed again.
Figure 2. Suicide attempts (SAs) incidence rate (100,000 person-months) in the East area of Valladolid, 2018-2023, estimated from Joinpoint regression analysis
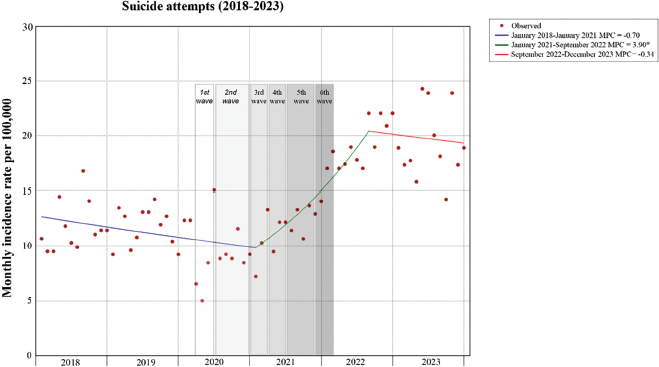
Note: *Indicates that the Monthly Percent Change (MPC) is significantly different from zero at the alpha = 0.05 level.
Focusing on the mean monthly incidence rates in the different years, Table 1 shows that in 2018 the MMIR SAs is 11.7 per 100,000 persons, decreasing in the following two years and starting to grow in 2021 until reaching a rate of 19.2 in 2023, producing an increase of 63.2% in the years analyzed.
Therefore, the set of results shows two distinct patterns: on the one hand, there is a trend toward stability in SDs, which do not vary significantly over time. On the other hand, the analyses reflect significant changes in SAs trends from pre-pandemic to post-pandemic years. When the pandemic begins in Spain (year 2020), a previous downward trend is observed, which is maintained during the first year of the pandemic. From this moment on, the SAs rate begins to increase, and a significant change occurs. This upward trend is maintained until a few months after the end of the pandemic, when cases begin to stabilize with a slight downward trend.
DISCUSSION
Clinical research shows that the problem of suicide is complex and multifactorial. A thorough understanding of the associated risk factors and the different variables involved is essential for establishing effective prevention policies (Mann et al., 2005). The recent pandemic has affected people’s lives, causing health, economic, and emotional problems. The population developed concern and fear about the possibility of becoming infected, reducing their income and losing their jobs, as well as the long-term consequences of the pandemic. The uncontrollability of the threat, its invisible nature, and the lack of information could facilitate the development of psychological problems (Sandín et al., 2020). The increase in mental health problems during the COVID-19 pandemic, mainly anxiety and depression, has led to more people being at increased risk. The World Health Organization (WHO) has repeatedly warned of the need to be prepared for future pandemics, and the latter represents an opportunity to learn (Taylor, 2022).
The present study has analyzed the evolution of trends in suicide deaths (SDs) and suicide attempts (SAs) during the last few years, focusing on the possible influence of the COVID-19 pandemic, so we included in this analysis the years before and after the pandemic in order to obtain a broader view. A critical aspect of our study that differentiates it from others conducted in our country is that we report data for the pre- and post-pandemic periods, which allows us to have a broader view when analyzing trends in suicide behaviors and the possible influence that the recent pandemic had on them. This longitudinal approach that includes different relevant periods, coupled with joinpoint regression analyses, brings a novel approach to the study of trends in suicide behaviors.
Consistently with other studies conducted in Spain (Hernández-Calle et al., 2020; Gómez-Revuelta et al., 2024), our data show that in the first months of the COVID-19 pandemic there was a reduction in SAs. This reduction was followed by a subsequent increase, a pattern that has been described in studies performed in other regions of Spain (Gómez-Revuelta et al., 2024; Pérez et al., 2022), as well as in meta-analyses that gather data from different countries (Yan et al., 2023). In the same way, an increase in the number of psychiatric consultations in the emergency service during the post-pandemic period has been reported in Spain, with a notable rise in problems related to anxiety, suicidal ideation, and self-harm (Aymerich et al., 2024). In the case of SDs, our data show that there was no significant change during the COVID-19 pandemic, a pattern that has also been found in a large part of the studies conducted in Europe (Lantos & Nyári, 2024) and in the rest of the world (da Cunha Varella et al., 2024; Pirkis et al., 2022). However, an increase in SDs has been reported in Spain (de la Torre et al., 2024). These divergences with our findings could be due to two causes: on the one hand, in our study we have only used data from the province of Valladolid, so that geographical variability could be a relevant variable. On the other hand, compared to the use of data from the Spanish National Statistics Institute (INE), in our study we have used data provided by the Institute of Legal Medicine of Valladolid, as we consider these data to be more accurate due to the possible underestimation of deaths by suicide in the INE data (Giner & Guija, 2014). Moreover, the increase in SDs has not only been found in Spain, but a similar pattern has been observed in other countries such as Japan (Tanaka & Okamoto, 2021) and in cities such as Mexico City (García-Dolores, 2023), so it should be emphasized that there are differences between different places in the world.
With a few exceptions, the findings indicate that there has not been a pattern of widespread increase in suicide deaths during the recent pandemic. Among the possible reasons most often cited in the literature are the following (da Cunha et al., 2024): economic support provided by the governments to mitigate the negative effects of lockdown and temporary company closures; the strengthening of family, friendship, and community bonds (social cohesion); and the decrease in stress and pressure related to the reconciliation of work and family life thanks to telecommuting. Nevertheless, given the well-established association between SAs and SDs, it would be relevant to analyze which variables could explain the fact that SAs have increased while SDs have remained stable.
During the first months of the pandemic, a downward trend in SAs continued. Although it may seem surprising, previous studies in other countries have found similar trends (Pirkis et al., 2021). It is reasonable to wonder whether the reduction in the number of persons attended in psychiatric emergency departments for SAs during the first months of the pandemic might be related to the strict lockdown measures. The fact is that an initial reduction in psychiatric emergency consultations has been documented in several countries (Ambrosetti et al., 2021; Balestrieri et al., 2021; Pignon et al., 2020), including Spain (Aymerich et al., 2024; Hernández-Calle et al., 2020). It is difficult to isolate the influence of containment measures to draw conclusions; however, in this period there was not only a decrease in the number of psychiatric emergency visits but also a reduction in the desire to die that has been reported (Cobo et al., 2021), so although these measures could be an influential factor, especially in the early months, they do not seem to explain the observed data alone.
Crisis situations have an impact on people’s mental health (Xiong et al., 2020), but this impact does not inevitably lead to an increase in suicides (Claassen et al., 2010; Kessler et al., 2006; Osman & Parnell, 2015). Many risk factors have been identified as influencing the impact of these events, with five main categories standing out: prior psychiatric hospitalization, prior suicide attempt, prior suicide ideation, socioeconomic status, and stressful life events (Franklin et al., 2017). In terms of protective factors, a tendency of communities to work together and support each other during crises has been described, a behavioral pattern referred to as “pulling together” (Gordon et al., 2011). When the circumstances are not conducive to its development, the results may be different. In this regard, loneliness was associated with increased depression and suicidal ideation at different times throughout the pandemic (Killgore et al., 2020).
As mentioned above, our findings show two distinct patterns: while SDs remained stable throughout the study period, unaffected by the beginning, development, and end of the pandemic, significant changes are observed in SAs influenced by this period of crisis, since while a downward trend was maintained at the beginning of the pandemic, as the months passed, these behaviors began to increase, reaching a peak in the final months of the pandemic and stabilizing after its end. It is important to note that we have observed a significant increase in SAs in 2022 and 2023. The reason for this variation is unknown, but analyzing the waiting times to receive care in the mental health service of the University Clinical Hospital of Valladolid, we found that they were significantly higher than in previous years. While in 2020, the year of the beginning of the pandemic, people received care, on average, in 38.4 days, in 2022 they received it in 74.4 days, which could explain the increase in visits to the emergency department, as well as an increase or worsening of mental health problems.
Over the years, different models have been proposed with the aim of explaining suicide behaviors (for a review, see Díaz-Oliván et al. 2021), including models that focus on different types of biological variables (e.g., Lutz et al., 2017), stress-diathesis models that propose an interaction between acute stressors —or proximal risk factors— and a diathesis —or distal risk factors— (e.g., Mann & Rizk, 2020), and interpersonal models that emphasize the relationships that the person develops with his or her social environment (e.g., Joiner, 2005). In general, these models try to explain suicide behaviors from a nomothetic approach. However, despite the usefulness of these models, as well as the identification of general risk and protective factors, the interaction of variables that lead to the emission of suicide behaviors is different in each person, so an idiographic level of analysis is required for a better understanding. The contextual perspective is framed at this level. From this approach, the spectrum of suicide behaviors (ideation, suicide attempt, and suicide death) would be conceptualized as a “pseudo-solution” to human suffering, that is, an escape from emotional pain rather than a tendency to end one’s life (Zaldívar et al., 2023). Some authors conceptualize suicide as an “existential drama” with two poles: the circumstance of life with its problems, conflicts, and dilemmas, and the choice of possibilities (González et al., 2021).
Suicide behavior coexists with and cuts across other mental health problems (Al-Halabí et al., 2021). However, in contrast to the attempt to explain it as a symptom of a disease or the product of a disorder, the contextual model proposes the need to analyze the behavior functionally, taking into account the person-context interaction and the analysis of the antecedents and consequents that control the behavior (Zaldívar et al., 2023). Suicide behaviors always make “sense” to the person, so in order to understand them, it is necessary to analyze the life history and the specific circumstances in which they are carried out. Within this framework, different contextual therapies such as Acceptance and Commitment Therapy (ACT) or Dialectical Behavior Therapy (DBT) have shown efficacy in reducing suicide behaviors (DeCou et al., 2019; Ducasse et al., 2018).
The findings shown in this study, together with the published literature on this topic, have significant implications for the management of suicide. Although suicide behaviors are a serious problem that should always keep us alert, in crisis situations such as the one that has occupied us with the COVID-19 pandemic, attention to this type of problem should be intensified, especially when the crisis situation is prolonged over time, due to the different factors that can influence the development of mental health problems (e.g., prolonged isolation, economic problems, etc.). In this sense, some measures implemented by governments, such as providing economic support to affected people, can alleviate the psychological impact in these crisis situations (Yao et al., 2022). Whether or not the statistics on suicide deaths have been affected by the pandemic, suicide continues to be a serious problem in the world. Any suicide death is already significant, so it is necessary to continue to learn about this problem in order to help people cope with problematic situations in the most effective way by finding alternative solutions. Given the large number of variables involved in suicide behaviors, it is essential to strengthen the public mental health system so that we can have the necessary resources to be able to develop individualized interventions that effectively address suicide behaviors.
Finally, it is worth mentioning that suicide has a stigma attached to it. There is often a perception that suicide behaviors represent a failure of the individual and the family to cope with some emotional problem (Cvinar, 2005), leading to feelings of guilt and social criticism of the survivors. In addition, two important implications have been pointed out: on the one hand, stigma can influence people to seek help for their problem, and on the other hand, stigma makes it difficult to obtain reliable data on the occurrence and characteristics of these behaviors (García-Haro et al., 2023). Therefore, interventions for the prevention and treatment of suicide behaviors should include specific actions aimed at addressing the problem of stigma.
LIMITATIONS AND FUTURE LINES OF RESEARCH
Data used for our analyses belong to two different samples, since while SAs are related to the population of the East Valladolid Health Area, SDs correspond to the total population of Valladolid. Likewise, the results obtained are relative to a specific area, and, although similar results have been found in other areas of Spain (Pérez et al., 2022; Gómez-Revuelta et al., 2024), they cannot be generalized to the whole country. Extending the sample to include data on SAs from the two health areas of Valladolid, and even from other provinces or autonomous communities, would make the results more reliable and would favor the development of comparative analyses between different geographical areas that would help to identify specific factors involved in suicide behavior.
The data on SAs are obtained from the psychiatric emergency register of the University Clinical Hospital of Valladolid. Especially during the months of confinement, it is possible that there were persons with thoughts of suicide and who even made an attempt at home who did not go to the emergency department, so that the data on SAs in the population as a whole are probably higher.
The study is mainly developed around joinpoint analysis, but in order to complement the results obtained, the use of other mean comparison tests could be relevant for future studies.
The COVID-19 pandemic had multiple effects on people’s lives, affecting their health, economy, social relations, or daily activity, so there is a long list of differentiated factors that have not been possible to control and that certainly play an important role in suicide behaviors. Although the evidence obtained to date is heterogeneous, including variables such as gender, age, or socioeconomic status, as well as their interaction, in the analysis of suicide behaviors trends could provide information on possible differences in the impact generated by the recent pandemic, as other studies have shown (Martínez-Alés et al., 2023).
CONCLUSIONS
Pandemics are complex events that can seriously affect people’s mental health, representing a risk factor for suicide behaviors. In the COVID-19 pandemic, we have observed that despite the impact on health and the economy and the influence on emotional problems, suicide deaths have not increased more than at other times. However, we found that as the months of the pandemic passed, there was an increase in suicide attempts, which is an indicator of mental health deterioration in the population. The findings highlight the need to strengthen mental health support in crisis situations, especially when these are prolonged over time.
Although the results are consistent with those found by other researchers in different parts of the world, it is important to mention that the study has some methodological and sample-related limitations. Future research should address these limitations by including variables such as gender, age, socioeconomic status, or loneliness in the analysis and by developing new lines of study with an idiographic approach to analyze the function that suicide behavior has in each case.
This crisis situation presents an opportunity to improve knowledge about the contextual and individual variables involved in suicide, as well as to learn from the measures and actions that have proven to be effective in combating its impact, both at the socioeconomic and health care levels, so that in future crisis situations we can pull together in the best possible conditions.
ETHICAL CONSIDERATIONS
All procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees and with the Helsinki Declaration of 1975 and its updates. The data were treated with complete confidentiality, and the participants included cannot be identified, since neither name, surname, date of birth, nor medical record number or episode of care were included in the database.
FUNDING
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
DECLARATION OF INTEREST STATEMENT
The authors declare that there are no conflicts of interest.
ACKNOWLEDGMENTS
This study was made possible by the collaboration of the Psychiatry department of the University Clinical Hospital of Valladolid and the Institute of Legal Medicine of Valladolid.
REFERENCES
Al-Halabí, Susana, & Fonseca-Pedrero, Eduardo. (2021). Suicidal behavior prevention: The time to act is now. Clínica y Salud, 32(2), 89–92. https://doi.org/10.5093/clysa2021a17
Al-Halabí, Susana; García-Haro, Juan; Rodríguez-Muñoz, María de la Fe, & Fonseca-Pedrero, Eduardo. (2021). Conducta suicida y periodo perinatal: entre el tabú y la incomprensión. Papeles del Psicólogo, 42(3), 161–169. https://doi.org/10.23923/pap.psicol.2963
Ambrosetti, Julia; Macheret, Laura; Folliet, Aline; Wullschleger, Alexandre; Amerio, Andrea; Aguglia, Andrea; Serafini, Gianluca; Prada, Paco; Kaiser, Stefan; Bondolfi, Guido; Sarasin, François, & Costanza, Alessandra. (2021). Impact of the COVID-19 pandemic on psychiatric admissions to a large Swiss emergency department: an observational study. International Journal of Environmental Research and Public Health, 18(3), 1174. https://doi.org/10.3390/ijerph18031174
Aymerich, Claudia; Pedruzo, Borja; Salazar de Pablo, Gonzalo; Olazabal, Nora; Catalan, Ana, & González-Torres, Miguel Ángel. (2024). Number and nature of psychiatric emergency department visits in a tertiary hospital before, during, and after coronavirus pandemic. Frontiers in Psychiatry, 15, 1380401. https://doi.org/10.3389/fpsyt.2024.1380401
Balestrieri, Matteo; Rucci, Paola; Amendola, Davide; Bonizzoni, Miki; Cerveri, Giancarlo; Colli, Chiara; Dragogna, Filippo; Ducci, Giuseppe; Elmo, Maria Giuseppa; Ghio, Lucio; Grasso, Federico; Locatelli, Clara; Mencacci, Claudio; Monaco, Leonardo; Nicotra, Alessandra; Piccinini, Giulia; Pischiutta, Livia; Toscano, Marco; Vaggi, Marco; Villari, Vincenzo; … Bondi, Emi. (2021). Emergency psychiatric consultations during and after the COVID-19 lockdown in Italy: A multicentre study. Frontiers in Psychiatry, 12, Article 697058. https://doi.org/10.3389/fpsyt.2021.697058
Cénat, Jude Mary; Blais-Rochette, Camille; Kokou-Kpolou, Cyrille Kossigan; Noorishad, Pari-Gole; Mukunzi, Joana N.; McIntee, Sara-Emilie; Dalexis, Rose Darly; Goulet, Marc-André, & Labelle, Patrick R. (2021). Prevalence of symptoms of depression, anxiety, insomnia, posttraumatic stress disorder, and psychological distress among populations affected by the COVID-19 pandemic: A systematic review and meta-analysis. Psychiatry Research, 295, 113599. https://doi.org/10.1016/j.psychres.2020.113599
Claassen, Cynthia A.; Carmody, Thomas; Stewart, Sunita M.; Bossarte, Robert M.; Larkin, Gregory L.; Woodward, Wayne A., & Trivedi, Madhukar H. (2010). Effect of 11 September 2001 terrorist attacks in the USA on suicide in areas surrounding the crash sites. The British Journal of Psychiatry, 196(5), 359–364. https://doi.org/10.1192/bjp.bp.109.071928
Cobo, Aurora; Porras-Segovia, Alejandro; Pérez-Rodríguez, María Mercedes; Artés-Rodríguez, Antonio; Barrigón, Maria Luisa; Courtet, Philippe, & Baca-García, Enrique. (2021). Patients at high risk of suicide before and during a COVID-19 lockdown: ecological momentary assessment study. BJPsych Open, 7(3), e82. https://doi.org/10.1192/bjo.2021.43
Cvinar, Jacqueline G. (2005). Do suicide survivors suffer social stigma: a review of the literature. Perspectives in Psychiatric Care, 41(1), 14–21. https://doi.org/10.1111/j.0031-5990.2005.00004.x
da Cunha Varella, Ana Paula; Griffin, Eve; Khashan, Ali, & Kabir, Zubair. (2024). Suicide rates before and during the COVID-19 pandemic: a systematic review and meta-analysis. Social Psychiatry and Psychiatric Epidemiology, 59(11), 1897–1905. https://doi.org/10.1007/s00127-024-02617-1
DeCou, Christopher R.; Comtois, Katherine Anne, & Landes, Sara J. (2019). Dialectical behavior therapy is effective for the treatment of suicidal behavior: A meta-analysis. Behavior Therapy, 50(1), 60–72. https://doi.org/10.1016/j.beth.2018.03.009
de la Torre-Luque, Alejandro; Perez-Diez, Ivan; Pemau, Andrés; Martinez-Ales, Gonzalo; Borges, Guilherme; Perez-Sola, Víctor, & Ayuso-Mateos, José Luis. (2024). Suicide mortality in Spain during the COVID-19 pandemic: Longitudinal analysis of sociodemographic factors. European Neuropsychopharmacology, 82, 29–34. https://doi.org/10.1016/j.euroneuro.2024.02.006
Díaz-Oliván, Isaac; Porras-Segovia, Alejandro; Barrigón, María Luisa; Jiménez-Muñoz, Laura, & Baca-García, Enrique. (2021). Theoretical models of suicidal behaviour: A systematic review and narrative synthesis. The European Journal of Psychiatry, 35(3), 181–192. https://doi.org/10.1016/j.ejpsy.2021.02.002
Ducasse, Déborah; Jaussent, Isabelle; Arpon-Brand, Véronique; Vienot, Marina; Laglaoui, Camelia; Béziat, Séverine; Calati, Raffaella; Carrière, Isabelle; Guillaume, Sébastien; Courtet, Philippe, & Olié, Emilie. (2018). Acceptance and commitment therapy for the management of suicidal patients: A randomized controlled trial. Psychotherapy and Psychosomatics, 87(4), 211–222. https://doi.org/10.1159/000488715
Fouillet, Anne; Martin, Diane; Pontais, Isabelle; Caserio-Schönemann, Céline, & Rey, Grégoire. (2023). Reactive surveillance of suicides during the COVID-19 pandemic in France, 2020 to March 2022. Epidemiology and Psychiatric Sciences, 32, e20. https://doi.org/10.1017/S2045796023000148
Franklin, Joseph C.; Ribeiro, Jessica D.; Fox, Kathryn R.; Bentley, Kate H.; Kleiman, Evan M.; Huang, Xieyining; Musacchio, Katherine M.; Jaroszewski, Adam C.; Chang, Bernard P., & Nock, Matthew K. (2017). Risk factors for suicidal thoughts and behaviors: A meta-analysis of 50 years of research. Psychological Bulletin, 143(2), 187–232. https://doi.org/10.1037/bul0000084
García-Dolores, Fernando; Tendilla-Beltrán, Hiram; Flores, Francisco; Carbajal-Rimoldi, Linda Alejandra; Mendoza-Morales, Roberto Cuauhtémoc; Gómez-Mendoza, Laura Endira; Vázquez-Hernández, Andrea Judith; de la Cruz, Fidel; Genis-Mendoza, Alma Delia; Nicolini, Humberto, & Flores, Gonzalo. (2023). Increased suicide rates in Mexico City during the COVID-19 pandemic outbreak: An analysis spanning from 2016 to 2021. Heliyon, 9(6), e16420. https://doi.org/10.1016/j.heliyon.2023.e16420
García-Haro, Juan; González, Marta G.; Fonseca-Pedrero, Eduardo, & Al-Halabí, Susana. (2023). Conceptualización de la conducta suicida. In Susana Al-Halabí, & Eduardo Fonseca-Pedrero (Coords.), Manual de psicología de la conducta suicida (pp. 31–68). Editorial Pirámide.
Giner, Lucas, & Guija, Julio A. (2014). Número de suicidios en España: diferencias entre los datos del Instituto Nacional de Estadística y los aportados por los Institutos de Medicina Legal [Number of suicides in Spain: differences between data from the Spanish Statistical Office and the Institutes of Legal Medicine]. Revista de Psiquiatria y Salud Mental, 7(3), 139–146. https://doi.org/10.1016/j.rpsm.2014.01.002
Gómez-Revuelta, Marcos; Sánchez-Lafuente, Carlos G.; Yáñez, Javier S.; Pindado, Luis Mariano G.; Echevarría, Luisa Elvira S. E.; Meseguer, Telva C.; Ruiz, Elsa G.; Bourgon, Javier V.; Simón, Jesús Ángel A.; Díaz, Ana Isabel S., & Terán, José María P. (2024). Long-term COVID-19 pandemic impact on suicide thoughts and behaviors (STB): An interrupted time series analysis in Spain 2-year after pandemic outbreak. Psychiatry Research, 339, 116086. https://doi.org/10.1016/j.psychres.2024.116086
González, Marta G.; García-Haro, Juan M.; García-Pascual, Henar; Pérez, Mónica T. S.; Barrio-Martínez, Sara, & Oviedo, Jairo V. (2021). Hacia un enfoque contextual-existencial del suicidio: recomendaciones para la prevención. Clínica Contemporánea, 12(1), e1. https://doi.org/10.5093/cc2021a3
González-Sanguino, Clara; Ausín, Berta; Castellanos, Miguel Ángel; Saiz, Jesús; López-Gómez, Aída; Ugidos, Carolina, & Muñoz, Manuel. (2020). Mental health consequences during the initial stage of the 2020 coronavirus pandemic (COVID-19) in Spain. Brain, Behavior, and Immunity, 87, 172–176. https://doi.org/10.1016/j.bbi.2020.05.040
Gordon, Kathryn H.; Bresin, Konrad; Dombeck, Joseph; Routledge, Clay, & Wonderlich, Joseph A. (2011). The impact of the 2009 Red River flood on interpersonal risk factors for suicide. Crisis, 32(1), 52–55. https://doi.org/10.1027/0227-5910/a000051
Hernández-Calle, Daniel; Martínez-Alés, Gonzalo; Mediavilla, Roberto; Aguirre, Pablo; Rodríguez-Vega, Beatriz, & Bravo-Ortiz, María Fe. (2020). Trends in psychiatric emergency department visits due to suicidal ideation and suicide attempts during the COVID-19 pandemic in Madrid, Spain. The Journal of Clinical Psychiatry, 81(5), 20l13419. https://doi.org/10.4088/JCP.20l13419
Instituto Nacional de Estadística. (n. d.). Defunciones por causas (lista detallada) sexo y edad. 2018-2023. Retrieved April 28, 2024, from https://www.ine.es/dyngs/INEbase/es/operacion.htm?c=Estadistica_C&cid=1254736176780&menu=resultados&idp=1254735573175#_tabs-1254736194710
Joiner, Thomas. (2005). Why people die by suicide. Harvard University Press.
Joinpoint Regression Program, Version 5.0.2. (2023, May). Statistical methodology and applications branch, surveillance research program, National Cancer Institute. https://surveillance.cancer.gov/joinpoint/
Kessler, Ronald C.; Galea, Sandro; Jones, Russell T.; Parker, Holly A., & Hurricane Katrina Community Advisory Group. (2006). Mental illness and suicidality after Hurricane Katrina. Bulletin of the World Health Organization, 84(12), 930–939. https://doi.org/10.2471/blt.06.033019
Killgore, William D. S.; Cloonan, Sara A.; Taylor, Emily C., & Dailey, Natalie. S. (2020). Loneliness: A signature mental health concern in the era of COVID-19. Psychiatry Research, 290, 113117. https://doi.org/10.1016/j.psychres.2020.113117
Kim, Hyune-Ju; Fay, Michael P.; Feuer, Eric J., & Midthune, Douglas. N. (2000). Permutation tests for joinpoint regression with applications to cancer rates. Statistics in Medicine, 19(3), 335–351. https://doi.org/10.1002/(sici)1097-0258(20000215)19:3<335::aid-sim336>3.0.co;2-z
Kõlves, Kairi; Kõlves, Keili E., & De Leo, Diego. (2013). Natural disasters and suicidal behaviours: a systematic literature review. Journal of Affective Disorders, 146(1), 1–14. https://doi.org/10.1016/j.jad.2012.07.037
Lantos, Tamás, & Nyári, Tibor András. (2024). The impact of the first year of COVID-19 pandemic on suicides in a collection of 27 EU-related countries. Scientific Reports, 14(1), 17671. https://doi.org/10.1038/s41598-024-68604-3
Lee, Yena; Lui, Leanna M. W.; Chen-Li, David; Liao, Yuhua; Mansur, Rodrigo B.; Brietzke, Elisa; Rosenblat, Joshua D.; Ho, Roger; Rodrigues, Nelson B.; Lipsitz, Orly; Nasri, Flora; Cao, Bing; Subramaniapillai, Mehala; Gill, Hartej; Lu, Ciyong, & McIntyre, Roger S. (2021). Government response moderates the mental health impact of COVID-19: A systematic review and meta-analysis of depression outcomes across countries. Journal of Affective Disorders, 290, 364–377. https://doi.org/10.1016/j.jad.2021.04.050
Lutz, Pierre E.; Mechawar, Naguib, & Turecki, Gustavo. (2017). Neuropathology of suicide: recent findings and future directions. Molecular Psychiatry, 22(10), 1395–1412. https://doi.org/10.1038/mp.2017.141
Mann, John J.; Apter, Alan; Bertolote, Jose; Beautrais, Annette; Currier, Dianne; Haas, Ann; Hegerl, Ulrich; Lonnqvist, Jouko; Malone, Kevin; Marusic, Andrej; Mehlum, Lars; Patton, George; Phillips, Michael; Rutz, Wolfgang; Rihmer, Zoltan; Schmidtke, Armin; Shaffer, David; Silverman, Morton; Takahashi, Yoshimoto; Varnik, Airi; … Hendin, Herbert. (2005). Suicide prevention strategies: a systematic review. JAMA, 294(16), 2064–2074. https://doi.org/10.1001/jama.294.16.2064
Mann, John J., & Rizk, Mina M. (2020). A brain-centric model of suicidal behavior. The American Journal of Psychiatry, 177(10), 902–916. https://doi.org/10.1176/appi.ajp.2020.20081224
Martínez-Alés, Gonzalo; Szmulewicz, Alejandro; López-Cuadrado, Teresa; Morrison, Christopher N.; Keyes, Katherine M., & Susser, Ezra S. (2023). Suicide following the COVID-19 pandemic outbreak: variation across place, over time, and across sociodemographic groups. A systematic integrative review. Current Psychiatry Reports, 25(7), 283–300. https://doi.org/10.1007/s11920-023-01427-7
Osman, Mugtaba, & Parnell, Andrew C. (2015). Effect of the First World War on suicide rates in Ireland: an investigation of the 1864-1921 suicide trends. BJPsych Open, 1(2), 164–165. https://doi.org/10.1192/bjpo.bp.115.000539
Ozamiz-Etxebarria, Naiara; Idoiaga Mondragon, Nahia; Dosil Santamaría, María, & Picaza Gorrotxategi, Maitane. (2020). Psychological symptoms during the two stages of lockdown in response to the COVID-19 outbreak: An investigation in a sample of citizens in northern Spain. Frontiers in Psychology, 11, 1491. https://doi.org/10.3389/fpsyg.2020.01491
Pérez, Víctor; Elices, Matilde; Vilagut, Gemma; Vieta, Eduard; Blanch, Jordi; Laborda-Serrano, E.; Prat, Bibiana; Colom, Francesc; Palao, Diego, & Alonso, Jordi. (2022). Suicide-related thoughts and behavior and suicide death trends during the COVID-19 in the general population of Catalonia, Spain. European Neuropsychopharmacology, 56, 4–12. https://doi.org/10.1016/j.euroneuro.2021.11.006
Pignon, Baptiste; Gourevitch, Raphaël; Tebeka, Sarah; Dubertret, Caroline; Cardot, Hélène; Dauriac-Le Masson, Valérie; Trebalag, Anne-Kristelle; Barruel, David; Yon, Liova; Hemery, François; Loric, Marie; Rabu, Corentin; Pelissolo, Antoine; Leboyer, Marion; Schürhoff, Franck, & Pham-Scottez, Alexandra. (2020). Dramatic reduction of psychiatric emergency consultations during lockdown linked to COVID-19 in Paris and suburbs. Psychiatry and Clinical Neurosciences, 74(10), 557–559. https://doi.org/10.1111/pcn.13104
Pirkis, Jane; Gunnell, David; Shin, Sangsoo; Del Pozo-Banos, Marcos; Arya, Vikas; Aguilar, Pablo A.; Appleby, Louis; Arafat, S. M. Yasir; Arensman, Ella; Ayuso-Mateos, Jose Luis; Balhara, Yatan P. S.; Bantjes, Jason; Baran, Anna; Behera, Chittaranjan; Bertolote, Jose; Borges, Guilherme; Bray, Michael; Brečić, Petrana; Caine, Eric; Calati, Raffaella; … Spittal, Matthew J. (2022). Suicide numbers during the first 9-15 months of the COVID-19 pandemic compared with pre-existing trends: An interrupted time series analysis in 33 countries. EClinicalMedicine, 51, 101573. https://doi.org/10.1016/j.eclinm.2022.101573
Pirkis, Jane; John, Ann; Shin, Sangsoo; DelPozo-Banos, Marcos; Arya, Vikas; Analuisa-Aguilar, Pablo; Appleby, Louis; Arensman, Ella; Bantjes, Jason; Baran, Anna; Bertolote, Jose M.; Borges, Guilherme; Brečić, Petrana; Caine, Eric; Castelpietra, Giulio; Chang, Shu-Sen; Colchester, David; Crompton, David; Curkovic, Marko; Deisenhammer, Eberhard A.; … Spittal, Matthew J. (2021). Suicide trends in the early months of the COVID-19 pandemic: an interrupted time-series analysis of preliminary data from 21 countries. The Lancet Psychiatry, 8(7), 579–588. https://doi.org/10.1016/S2215-0366(21)00091-2
Radeloff, Daniel; Genuneit, Jon, & Bachmann, Christian J. (2022). Suicides in Germany during the COVID-19 pandemic. Deutsches Arzteblatt International, 119(29-30), 502–503. https://doi.org/10.3238/arztebl.m2022.0198
Ramos, Sara Freitas; Vaz Soares, Mafalda Isabel Fonseca Marinho; Correia, João Martins; Jesus, Bianca; Cruz e Sousa, Diana, & Mendes, João. (2021). The impact of COVID-19 pandemic on suicides in Portugal during the emergency state. European Psychiatry, 64(Suppl 1), S95. https://doi.org/10.1192/j.eurpsy.2021.279
Ribeiro, Jessica D.; Franklin, Joseph C.; Fox, Kathryn R.; Bentley, Kate H.; Kleiman, Evan M.; Chang, Bernard P., & Nock, Matthew. K. (2016). Self-injurious thoughts and behaviors as risk factors for future suicide ideation, attempts, and death: a meta-analysis of longitudinal studies. Psychological Medicine, 46(2), 225–236. https://doi.org/10.1017/S0033291715001804
Sandín, Bonifacio; Valiente, Rosa M.; García-Escalera, Julia; Campagne, Daniel M., & Chorot, Paloma. (2020). Psychological impact of the COVID-19 pandemic: Negative and positive effects in Spanish population during the mandatory national quarantine. Revista de Psicopatología y Psicología Clínica, 25(1), 1e–21e. https://doi.org/10.5944/rppc.28107
Tanaka, Takanao, & Okamoto, Shohei. (2021). Increase in suicide following an initial decline during the COVID-19 pandemic in Japan. Nature Human Behaviour, 5(2), 229–238. https://doi.org/10.1038/s41562-020-01042-z
Taylor, Steven. (2022). The psychology of pandemics. Annual Review of Clinical Psychology, 18, 581–609. https://doi.org/10.1146/annurev-clinpsy-072720-020131
Turecki, Gustavo; Brent, David A.; Gunnell, David; O’Connor, Rory C.; Oquendo, Maria A.; Pirkis, Jane, & Stanley, Barbara H. (2019). Suicide and suicide risk. Nature Reviews Disease Primers, 5(1), 74. https://doi.org/10.1038/s41572-019-0121-0
World Health Organization. (2021). Suicide worldwide in 2019: global health estimates. https://www.who.int/publications/i/item/9789240026643
Xiong, Jiaqi; Lipsitz, Orly; Nasri, Flora; Lui, Leanna M. W.; Gill, Hartej; Phan, Lee; Chen-Li, David; Iacobucci, Michelle; Ho, Roger; Majeed, Amma, & McIntyre, Roger S. (2020). Impact of COVID-19 pandemic on mental health in the general population: a systematic review. Journal of Affective Disorders, 277, 55–64. https://doi.org/10.1016/j.jad.2020.08.001
Yan, Yifei; Hou, Jianhua; Li, Qing, & Yu, Nancy Xiaonan. (2023). Suicide before and during the COVID-19 pandemic: A systematic review with meta-analysis. International Journal of Environmental Research and Public Health, 20(4), 3346. https://doi.org/10.3390/ijerph20043346
Yao, Haitang; Wang, Jiayang, & Liu, Wei. (2022). Lockdown policies, economic support, and mental health: Evidence from the COVID-19 pandemic in United States. Frontiers in Public Health, 10, 857444. https://doi.org/10.3389/fpubh.2022.857444
Zaldívar, Flor; López-Ríos, Francisca, & García-Montes, José Manuel. (2023). Modelos psicológicos en la conducta suicida. In Susana Al-Halabí, & Eduardo Fonseca-Pedrero (Coords.), Manual de psicología de la conducta suicida (pp. 69–110). Editorial Pirámide.

LUIS SOBRINO CONDE
Psychology graduate from the Autonomous University of Madrid. He holds Master’s degrees in Clinical Psychology, Neuroscience, and Forensic Sciences. Currently, he is a Clinical Psychology Resident at the Hospital Clínico Universitario de Valladolid and a PhD student at the University of Valladolid.
lsobrinoc@saludcastillayleon.es
https://orcid.org/0009-0004-7609-8259
ANA ISABEL SEGURA RODRÍGUEZ
Specialist in Clinical Psychology and supervisor for PIR residents at the Hospital Clínico Universitario de Valladolid. She is the author of several publications, including Desarrollo psicoafectivo y psicopatología: salud mental y condición humana (2022).
asegurar@saludcastillayleon.es
https://orcid.org/0009-0005-2145-1702
JOSÉ ANTONIO BLANCO GARROTE
Psychiatrist at the Hospital Clínico Universitario de Valladolid. He holds a PhD from the University of Valladolid, specializing in dementia and cognitive impairment research among the institutionalized elderly, including the validation of the Mini-Mental State Examination (MEC).
joseantonio.blanco@uva.es
https://orcid.org/0000-0003-1304-8137
CITATION
Sobrino-Conde, Luis; Segura-Rodríguez, Ana Isabel, & Blanco-Garrote, José Antonio. (2026). Trends in Suicide Behaviors in Valladolid During the COVID-19 Pandemic (2018-2023). Quaderns de Psicologia, 28(1), e2219. https://doi.org/10.5565/rev/qpsicologia.2219
EDITORIAL HISTORY
Received:1-09-2024
1st revision: 30-01-2025
2nd revision: 1-04-2025
Accepted: 14-04-2025
Published: 25-04-2026